NRG1: It’s more aggressive than you think

NRG1 fusions are emerging drivers in tumors linked to aggressive features and poor clinical outcomes1-3
Discover how NRG1
fusions drive tumor growth
NRG1 across tumor types
NRG1 fusions have been identified across many solid tumor types and generally occur in the absence of other driver mutations1,4
NRG1 fusion frequency estimates
Overall (<1%)5,6
EnrichmentInvasive mucinous lung adenocarcinoma (up to 31%)7-9
Overall (<2%)5,10
EnrichmentKRAS wild-type pancreatic cancer (up to 3%)10,11
Overall (<1%)5
Breast, cholangiocarcinoma, colorectal, gallbladder, sarcoma, ovarian cancers, renal cell carcinoma, etc5
TEST YOUR KNOWLEDGE
Why should I be concerned about pathogenic gene fusions such as NRG1?

They are rare and not actionable

They only appear in select tumor types

Missing them can lead to poor outcomes
Metastatic potential
Studies observed that NRG1+ tumors possess aggressive histological features associated with increased tumor growth, invasiveness, recurrence, resistance to therapy, metastasis, and worse prognosis in lung cancer.3,7,8,a
NRG1+ tumors have a higher rate of metastasis at diagnosis compared with KRAS+ tumors (67% vs 32%, respectively)7

NRG1+ tumors are 10x more likely to have concurrent intra- and extrathoracic metastases than KRAS+ tumors (50% vs 5%, respectively)7
Most common sites of NRG1+ extrathoracic metastases in IMA1
0
0
0
Poor outcomes and therapeutic resistance
NRG1 fusions are associated with poor outcomes and resistance to therapies in lung cancer1,3
Activity of systemic
therapy in NRG1+ NSCLC1,b
therapy in NRG1+ NSCLC1,b

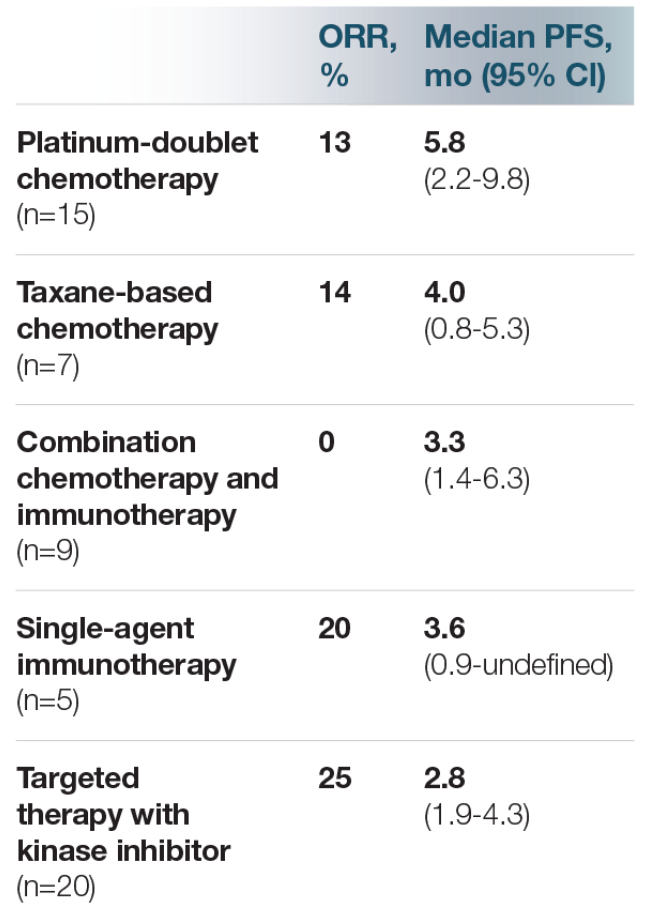
In a retrospective global registry study of 110 patients, NRG1+ NSCLC was associated with limited response to available therapies.1
NRG1+ cancers are associated with lower OS, DFS, and PFS.1,3,8
DFS, disease-free survival; IMA, invasive mucinous adenocarcinoma; NGS, next-generation sequencing; NRG1, neuregulin 1; NRG1+, neuregulin 1 fusion positive; NSCLC, non–small cell lung cancer; ORR, objective response rate; OS, overall survival; PFS, progression-free survival.
aIn a study by Chang et al (2021) at Memorial Sloan Kettering Cancer Center, histological slides from 200 IMAs were reviewed by 2 thoracic pathologists. Primary tumor size was measured pathologically in resected tumors and radiologically in unresected tumors. Presence of tumor necrosis and stromal invasion, defined by stromal desmoplasia surrounding invasive glands or nests of tumor cells, were recorded. Clinical outcomes data associated with these tumors were retrieved from electronic medical records.7 Shin et al (2016) tested 59 IMA samples obtained from patients who underwent curative surgical resection, identifying 13 SLC3A2-NRG1 fusions (27% frequency). Tumor xenografts in nude mice were generated for measuring tumor volume and weight. Proliferation, tumor volume, and weight were analyzed for cancer cells ectopically expressing SLC3A2, NRG1, and SLC3A2-NRG1.8
bPatients either diagnosed with or who developed metastatic disease during the course of their disease.
References: 1. Drilon A, Duruisseaux M, Han J-Y, et al. Clinicopathologic features and response to therapy of NRG1 fusion–driven lung cancers: the eNRGy1 Global Multicenter Registry. J Clin Oncol. 2021;39(25):2791-2802. doi:10.1200/JCO.20.03307 2. Laskin J, Liu SV, Tolba K, et al. NRG1 fusion-driven tumors: biology, detection, and the therapeutic role of afatinib and other ErbB-targeting agents. Ann Oncol. 2020;31(12):1693-1703. doi:10.1016/j.annonc.2020.08.2335 3. Rosas D, Raez LE, Russo A, Rolfo C. Neuregulin 1 gene (NRG1). A potentially new targetable alteration for the treatment of lung cancer. Cancers (Basel). 2021;13(20):5038. doi:10.3390/cancers13205038 4. Liu SV. Plain language summary of NRG1 fusions in cancer: current knowledge and treatment with afatinib and other drugs. Future Oncol. 2022;18(26):2865-2870. doi:10.2217/fon-2022-0073 5. Jonna S, Feldman RA, Swensen J, et al. Detection of NRG1 gene fusions in solid tumors. Clin Cancer Res. 2019;25(16):4966-4972. doi:10.1158/1078-0432.CCR-19-0160 6. Severson E, Achyut BR, Nesline M, et al. RNA sequencing identifies novel NRG1 fusions in solid tumors that lack co-occurring oncogenic drivers. J Mol Diagn. 2023;25(7):454-466. doi:10.1016/j.jmoldx.2023.03.011 7. Chang JC, Offin M, Falcon C, et al. Comprehensive molecular and clinicopathologic analysis of 200 pulmonary invasive mucinous adenocarcinomas identifies distinct characteristics of molecular subtypes. Clin Cancer Res. 2021;27(14):4066-4076. doi:10.1158/1078-0432.CCR-21-0423 8. Shin DH, Lee D, Hong DW, et al. Oncogenic function and clinical implications of SLC3A2-NRG1 fusion in invasive mucinous adenocarcinoma of the lung. Oncotarget. 2016;7(43):69450-69465. doi:10.18632/oncotarget.11913 9. Trombetta D, Graziano P, Scarpa A, et al. Frequent NRG1 fusions in caucasian pulmonary mucinous adenocarcinoma predicted by Phospho-ErbB3 expression. Oncotarget. 2018;9(11):9661-9671. doi:10.18632/oncotarget.23800 10. Knepper TC, Kim DW, Mauer E, Ronski K, Gulhati P. Comparative analysis of the targetable landscape in KRAS-mutant and wild-type pancreatic adenocarcinoma. Poster presented at: 2022 ASCO Annual Meeting; June 3-7, 2022; Chicago, IL. 11. Philip PA, Azar I, Xiu J, et al. Molecular characterization of KRAS wild-type tumors in patients with pancreatic adenocarcinoma. Clin Cancer Res. 2022;28(12):2704-2714. doi:10.1158/1078-0432.CCR-21-3581


